Juno recently released a TGA-approved pre-filled syringe containing metaraminol. However, not long after release, multiple issues were identified by anaesthetists who were using them. There was a fair bit of discussion and sharing of information and experiences on Twitter, and many anaesthetists have stopped using them, and some hospitals have now withdrawn them. Several people have contacted me regarding the syringes, and I thought I would aggregate some of the information I’ve collected in one place to make it easy for people to access it if they want to.
Tag: medication
Valvular Insufficiency
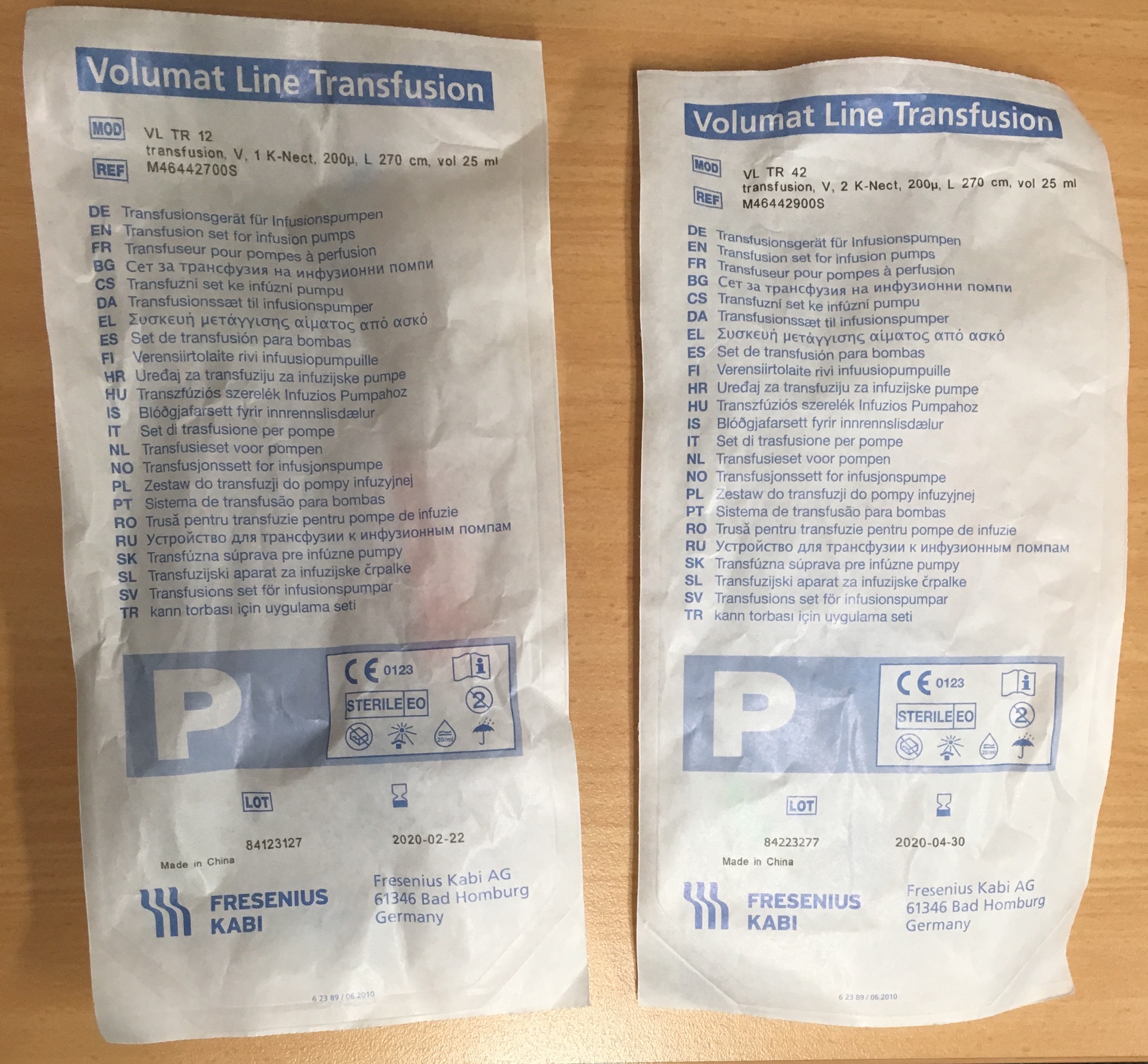
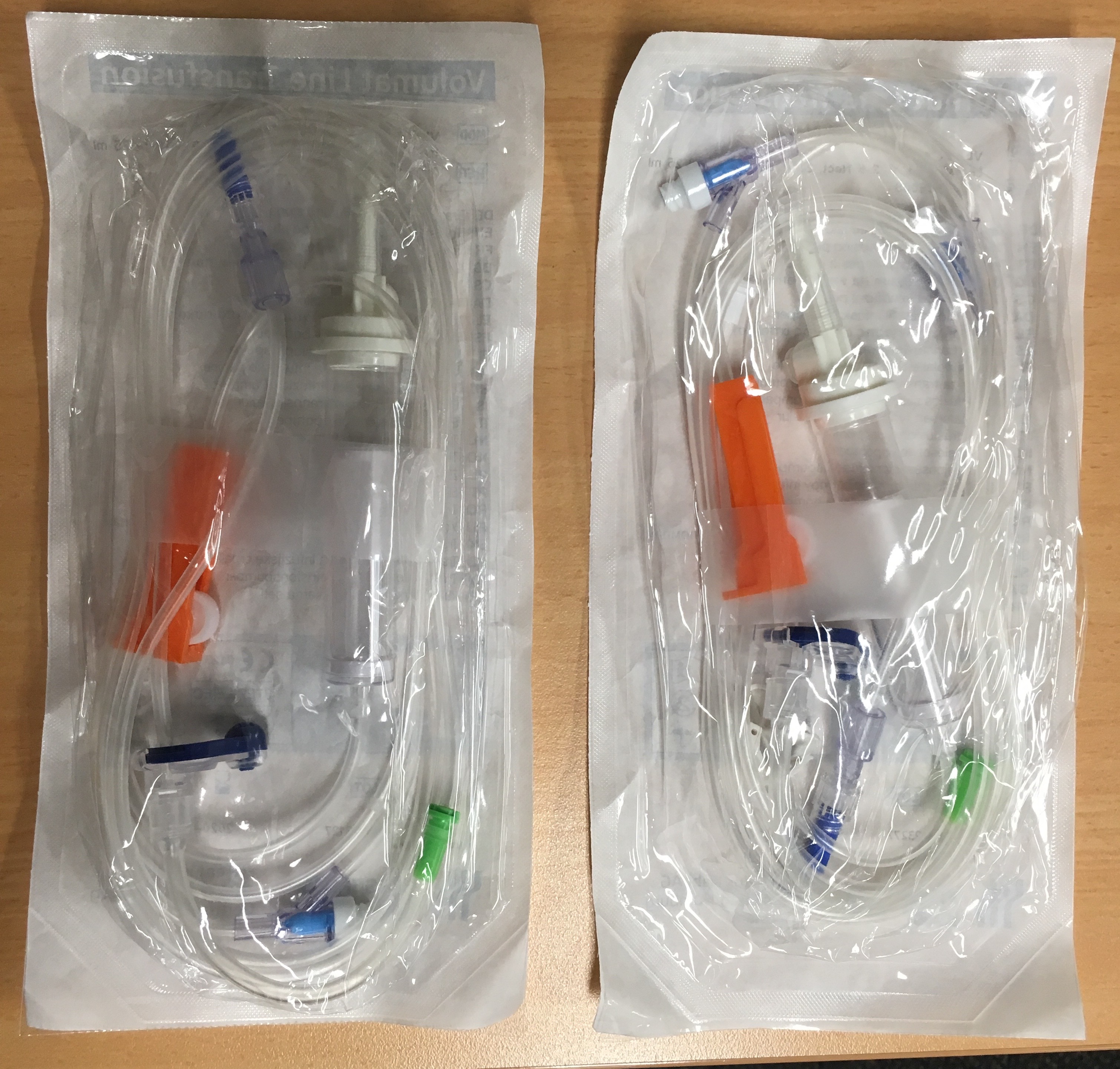
Take a look at the image below and see if you can spot the differences between these two IV giving sets:
Maybe the packaging will help?
How did you go? There are actually a few differences between them, but there is one in particular that I am interested in, and you should be too. Can you guess which one it is? Yes, that little white bit circled in red is what’s called a “one-way”, “back check” or 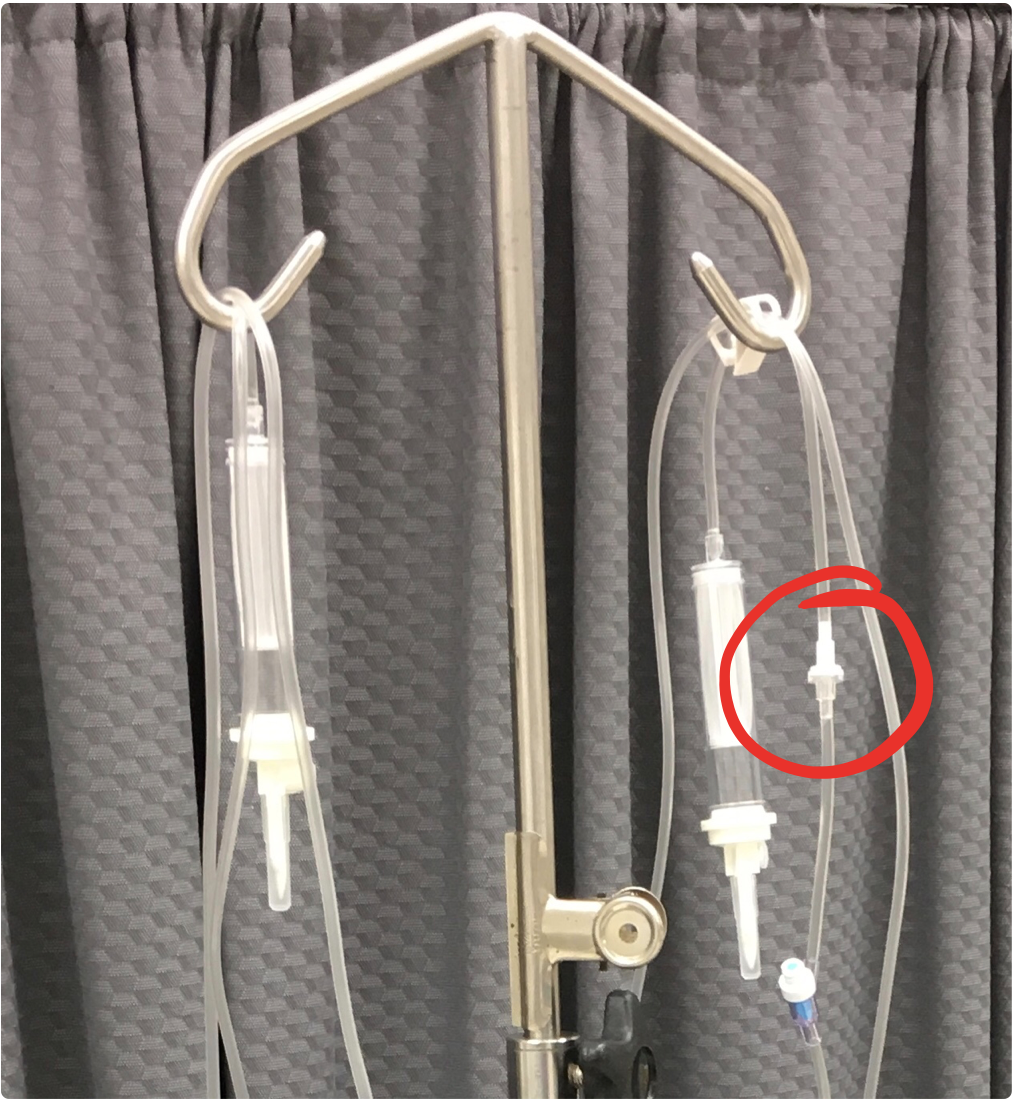 just “check” valve. As the name suggests it ensures fluid in the line can only move one-way i.e. from the IV fluid bag and into the patient. This valve is there so that if you are running a secondary infusion it will flow into the patient, rather than back up the primary line and into the fluid bag. A visual representation of what this valve does can be seen in this video:
just “check” valve. As the name suggests it ensures fluid in the line can only move one-way i.e. from the IV fluid bag and into the patient. This valve is there so that if you are running a secondary infusion it will flow into the patient, rather than back up the primary line and into the fluid bag. A visual representation of what this valve does can be seen in this video:
EHRs: Safety vs Privacy & the ETTO Principle
A little while back I posted about the challenges a family member faced after forgetting to bring their medications when they came to visit us. In that post, I referred to the Electronic Transfer of Prescriptions (eTP) and I’ve now taken a closer look at this system and discovered some useful features, but also significant room for improvement and expansion.
Continue reading “EHRs: Safety vs Privacy & the ETTO Principle”
Travelling, Medications and Patient Work
Edit 18/5/2018: A follow-up to this post can be found here.
My parents, as they often do, came up to Newcastle and stayed for a few nights last week, and it ended up being a case study in Patient Work.
My mother left all her medications at home. I’m sure she’s not the first, and won’t be the last person to make this kind of skill-based error known as a “lapse”, but it immediately raised some obvious questions and issues that she, and others, had to go about solving, requiring significant amounts of time and mental effort which all contributed to her Patient Workload. Continue reading “Travelling, Medications and Patient Work”
The Complexity of Patient Work: An Addendum
There’s been yet another twist in my earlier story about trip to Sydney for a medical appointment a little while back. I popped into my pharmacist earlier this week to get a script filled and he casually asked me if wanted my final lot of Humira, which was the medication I was driving all over Sydney to try and get because I had run out. As it turned out, I had one more repeat than I had thought, and the pharmacist had filled it expecting me to come back and get it when I needed. This meant there was more Humira sitting in the pharmacy fridge in Newcastle waiting for me the whole time I was going going back and forth across Sydney!
Sigh…
The Complexity of Patient Work
Following my recent “discovery” of the concept of Patient Work, it has reframed the way I view all my interactions with the healthcare system such as doctors visits, taking medication, blood tests and scans and so on. I’ve decided I’m going to start describing and documenting some of these interactions primarily for my own interest, but also in case others find them interesting as well. What follows is an almost textbook example of some of the complexity and unpredictability of Patient Work, and the need for the Patient Work System to be resilient enough to cope with these variations and uncertainties